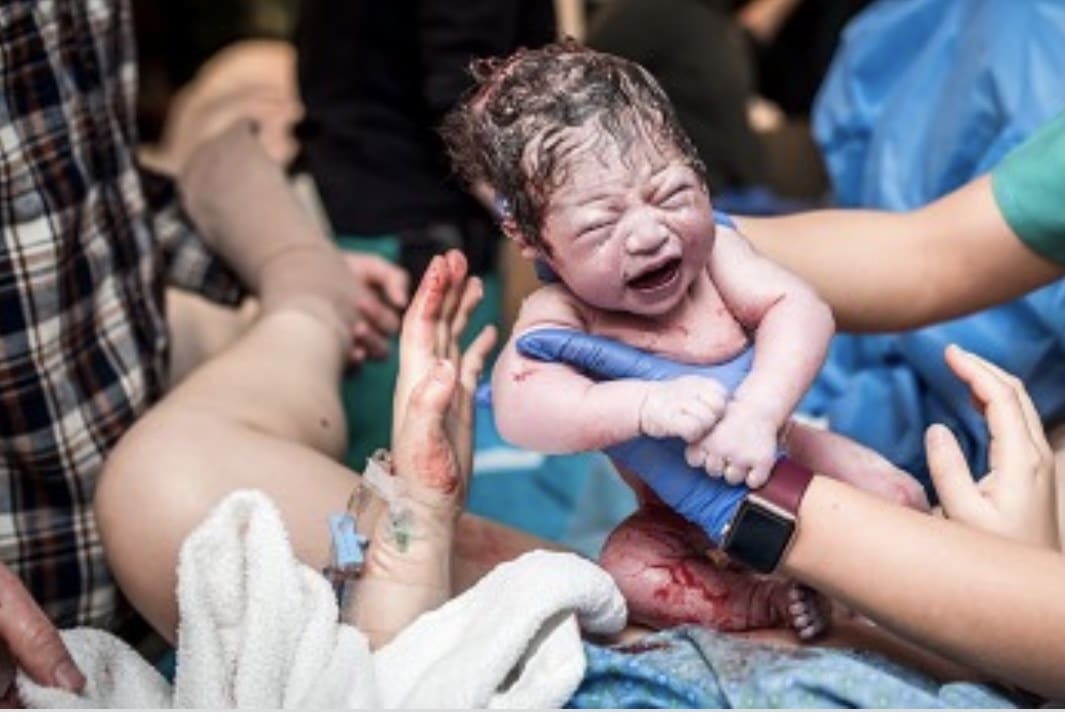
Childbirth - What you Need to Know
Childbirth is a transformative experience that brings joy and anticipation to expectant parents. However, it can also be accompanied by uncertainties and questions. Understanding the essential information and equipping oneself with helpful tips can help alleviate concerns and empower expectant parents on their journey towards childbirth. This article aims to provide valuable insights and guidance, covering key aspects of childbirth and offering tips to support a positive birthing experience.
1. Childbirth Preparation: Knowledge is Power
Preparing for childbirth involves acquiring the necessary knowledge about the process to make informed decisions and feel more confident. Familiarize yourself with the different stages of labor, the physical and emotional changes that occur, and pain management techniques. Attend childbirth education classes or workshops, read reputable resources, and engage with healthcare professionals to gain a comprehensive understanding of what to expect during childbirth.
2. Creating a Birth Plan: Tailoring Your Experience
Developing a birth plan allows expectant parents to articulate their preferences and desires for their birthing experience. Consider aspects such as location (hospital, birthing center, home), pain management options (natural techniques, medication), support persons, and any specific cultural or religious considerations. Discuss your birth plan with your healthcare provider to ensure it aligns with your medical needs and any potential complications.
3. Prenatal Care: Nurturing Your Health
Attending regular prenatal check-ups is crucial for monitoring the health of both the mother and the baby. These appointments provide an opportunity to address any concerns, track the growth and development of the fetus, perform necessary medical tests, and receive guidance on maintaining optimal health during pregnancy. Follow your healthcare provider’s recommendations regarding nutrition, exercise, and lifestyle habits to promote a healthy pregnancy and prepare for childbirth.
4. Pain Management Techniques: Exploring Your Options
Childbirth can be associated with varying levels of discomfort or pain. Educate yourself about the range of pain management techniques available. These include natural methods such as breathing techniques, relaxation exercises, hydrotherapy, and positions for labor. Additionally, familiarize yourself with medical interventions such as epidurals or analgesics. Discuss these options with your healthcare provider to determine the best approach for your specific needs.
5. Building a Support System: Emotionally Nurturing Reassurance
Surrounding yourself with a supportive network can make a significant difference during childbirth. Build a support system that includes your partner, family members, friends, or a doula, if desired. These individuals can provide emotional reassurance, physical support, and advocate for your preferences during labor. Communicate your needs and expectations to your support system, ensuring everyone is aligned in their understanding of your birth plan.
6. Postpartum Care: Transitioning to Parenthood
Transitioning to parenthood involves postpartum care and support. Understand the physical and emotional changes that occur after childbirth, including healing from delivery, establishing breastfeeding, and managing the emotional rollercoaster commonly referred to as the “baby blues.” Seek assistance and resources to assist with postpartum recovery and to navigate the challenges and joys of early parenthood.
By equipping yourself with essential information, preparing a birth plan, and building a support system, you can approach childbirth with confidence and positivity. Remember that each birthing experience is unique, and flexibility is key as unexpected circumstances may arise. By prioritizing your health, staying informed, and advocating for your preferences, you can contribute to a positive childbirth experience that welcomes your new arrival with joy and love.